Researchers at Cincinnati Children's have identified a cell that appears to be linked to life-threatening food allergies.
On tests using mice, the newly discovered cell produced large amounts of an inflammatory immune protein which amplified anaphylactic shock. Food is the most common cause of such shock.
The study author's say the findings could lead to new strategies for dealing with food allergies. It could also lead to new tests to determine if a patient is at a higher risk for food allergies.
The findings are reported in the September 22 issue of the journal Immunity.
What Researchers Found
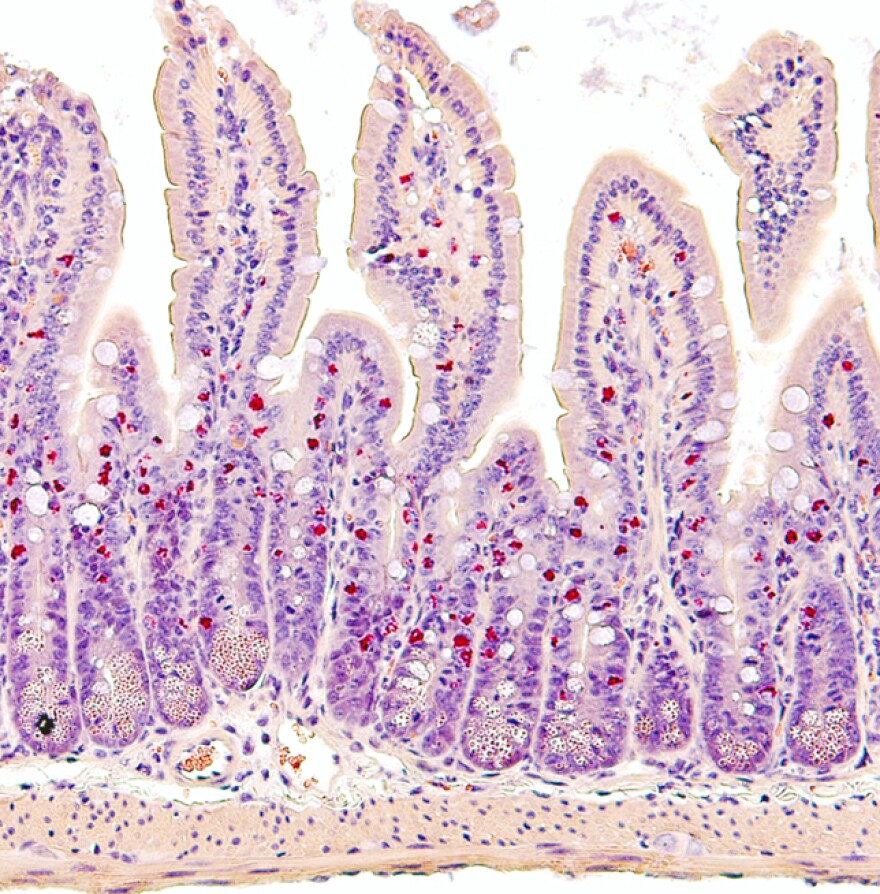
Anaphylactic shock related to food allergies is triggered by an immune antibody known as immunoglobulin E, or IgE. Researchers found mucosal mast cells (MMC9) which produce large amounts of an inflammatory immune protein called interlukin 9 (IL-9). This protein, in turn, boosts anaphylactic shock caused by a response to certain foods.
According to a news release:
"Our study suggests that although you need to have some level of IgE to trigger a food allergy response, you also have to produce MMC9 cells to get a severe response and anaphylaxis," says Yui-Hsi Wang, PhD, lead investigator and a researcher in the Division of Allergy and Immunology at Cincinnati Children's. "Without these cells you will not get severe food allergies."
Wang said the researchers are now trying to find the human equivalent (orthologue) of the MMC9 cells they found in their mouse models. One goal the researchers have is to identify that cell and its biological mediators to see if it possible to develop a biomarker that might allow development of a blood test for food allergies. Eventually, Wang said, the team wants to develop a blood test that would allow clinicians to determine which patients are at higher risk for severe food allergies, and to find improved treatments for food allergy. Also working with Wang on the study were co-first authors and Cincinnati Children's colleagues Chun-Yu Chen, PhD and Jee-Boong Lee, PhD the Division of Allergy and Immunology.



